Help Center
Online Resource Center for Information on Birth Injuries.
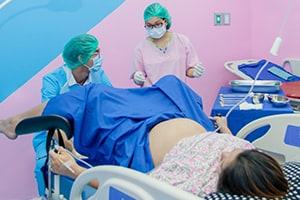
While most people think of labor and childbirth solely as the process of a child being born, most do not know or realize that the process is not complete when the child is born. Rather, the final stage of labor involves the placenta being expelled from the uterus after the birth has occurred. In most cases, this occurs automatically minutes after the baby has passed through the birth canal.
Retained placenta is an uncommon delivery complication (1-3% of live deliveries) that occurs when the placenta does not come out on its own but rather remains inside the womb after the baby comes out. If this occurs, doctors must intervene to manually manipulate the placenta out of the womb. Otherwise, if the placenta is left in the womb, a very serious and potentially fatal infection can develop.
When the placenta has not been expelled within 30 minutes after delivery it is diagnosed as retained placenta because the body has kept the placenta rather than expelling it in the normal time frame. If retained placenta goes untreated (i.e., the placenta is not removed), a woman becomes very susceptible to postpartum infection and potentially dangerous blood loss, both of which can very quickly become life-threatening.
There are several different types of retained placentas and they differ considerably in how they occur and the risks associated with them. Specifically, there are three classifications of placentas that are described below.
While any woman can experience a retained placenta, some factors increase the likelihood of experiencing one. For one, retained placentas are more common in women who become pregnant after they turn 30.
Additionally, premature deliveries occurring before the 34th gestational week can increase the risk as the placenta needs to remain in place until gestational weeks 34-40. Having a very long first and second stage of delivery can also increase the risk and be a sign you may experience one. Lastly, retained placentas are common in women who deliver a stillborn baby.
Removal of the placenta from the womb is the only treatment option for a retained placenta, however, there are different methods of manual removal. You can opt for an anesthetic and the OB/GYN can try to remove it manually, but the risk of infection is elevated.
Some medications can trigger additional contractions or relax the uterus muscles and help expel the placenta.
Breastfeeding causes the uterus to naturally contract which can sometimes be enough to expel it. Also, a full bladder can impede the placenta from expelling out of the womb. As a result, in some cases urinating actually can help effectively expel the placenta. When none of the above methods work to expel the placenta, in some cases emergency surgery is needed, although it is only used as a last resort as it carries a number of complications.
When it comes to a retained placenta, there are complications that may arise. For one, retained placentas can result in a primary postpartum hemorrhage resulting in excessive heavy internal bleeding.
While anesthetics can help during the delivery process, they can result in further risks particularly if you are planning to breastfeed immediately after the procedure. This is because your system will have traces of the drug within it which will pass those traces to your breastmilk.
You also want to ensure that when coming off an anesthetic you are alert enough to hold and support your baby. If you decide to opt for an anesthetic, however, the OB/GYN will manually remove the placenta and remaining membranes manually. Following the procedure, you will be prescribed antibiotics to mitigate the risk of infection while other drugs will be prescribed to help the womb contract.
Lekuikeu, L.S.T., & Moreland, C. (2022). Retained Placenta and Postpartum Hemorrhage: A Case Report and Review of Literature. Cureus, 14(4).
This case study and review looked at how a retained placenta increased the postpartum hemorrhage risk.
Favilli, A., et al. (2021). Risk factors for non-adherent retained placenta after vaginal delivery: a systematic review. BMC pregnancy and childbirth, 21(1), 1-13.
This study looked at a retained placenta’s risk factors. The researchers found that the retained placenta incidence ranged between 0.5 and 4.8 percent. They also found that the most recurrent risk factors were maternal age, prior C-section history, prior dilation and curettage history, prior retained placenta, and labor induction.
Kumar, N., et al. (2021). Umbilical vein injection for management of retained placenta. Cochrane Database of Systematic Reviews.
This study looked at whether umbilical vein injections would help manage a retained placenta. The researchers found that there was “low-certainty” evidence that injecting oxytocin would prevent the occurrence of a manual placenta removal. They also found that there were few differences in outcomes of other medications.
Granfors, M., et al. (2020). Placental location and risk of retained placenta in women with a previous cesarean section: A population‐based cohort study. Acta Obstetricia et Gynecologica Scandinavica, 99(12), 1666-1673.
The researchers found that the anterior placental location did not mediate the increased retained placenta risk in women with prior C-sections.
Patrick, H. S., et al. (2020). Pharmacologic intervention for the management of retained placenta: a systematic review and meta-analysis of randomized trials. American Journal of Obstetrics and Gynecology, 223(3), 447-e1.
This review and meta-analysis looked at whether pharmacologic interventions help manage a retained placenta. The researchers found that oxytocin via umbilical vein injections, nitroglycerin, and prostaglandin agents performed favorably compared to a placebo. They also found that prostaglandin and carbetocin agents performed better than oxytocin and reduced the need for dilation and curettage and manual extractions.
Perlman, N.C., et al. (2019). Retained placenta after vaginal delivery: risk factors and management. International Journal of Women’s Health, 11, 527-534. This article reported that the retained placenta period was variably defined between 18 and 60 minutes.
Endler, M., et al. (2018). The inherited risk of retained placenta: a population based cohort study. BJOG. 125(6), 737–744.
This study found that a retained placenta in the first generation significantly increased the risk of a retained placenta in the second.
Nikolajsen, S., et al. (2018). Reoccurrence of retained placenta at vaginal delivery: an observational study. Acta Obstet Gynecol Scand, 92(4), 421–425.
The study showed that the retained placenta occurrence ranged between 2.8 to 7 percent. It also underscored the increased reoccurrence risk in future vaginal deliveries.
Urner, F., et al. (2014). Manual removal of the placenta after vaginal delivery: an unsolved problem in obstetrics. J Pregnancy.
This study looked at the challenges of manually removing the placenta after a vaginal delivery.