Help Center
Online Resource Center for Information on Birth Injuries.
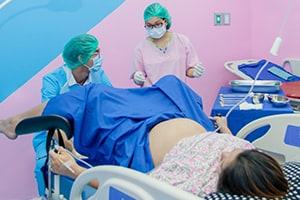
Giving birth is one of the most intense and painful experiences a woman will ever experience during her life, with or without an epidural. Pushing a 6 or 8-pound baby out of a small birth canal tests the physical limitations of the female body.
A typical labor and delivery can involve hours of pain from powerful uterine contractions, stretching, tearing, and pressure. This is why maternal pain management has become an important component of modern obstetric practice.
In recent years the epidural has become the predominant method of pain management for women in labor. An epidural is given for pain in over 71% of all hospital deliveries in the U.S.
Like all medications and procedures, the epidural has pros and cons. Intelligent women who love their unborn babies make different choices on whether to get an epidural. This page will give a brief overview of the good and the bad about epidurals during childbirth to help you make the right choice for you and your baby.
The term epidural refers to the process of administering regional anesthesia medication directly into the epidural space in the mother’s lower spine. The epidural space is an area that surrounds the spine and is filled with fluid. The nerve pathways which carry pain and other sensation from the brain to the lower body run through the spine area.
When a regional analgesic medication is injected directly into the epidural space, it blocks pain signals from going to the lower body through these nerve pathways. This makes the epidural a highly effective method of numbing the lower half of a mother’s body during labor. This significantly decreases the level of pain that the mother feels during labor and delivery. The exact type of drug or combination of drugs administered with an epidural varies.
An epidural during labor involves more than just a single injection of pain medication into the epidural space. One injection will not last long enough. So the anesthesiologist taps into the epidural space with a special needle that stays in place. It is attached to a drip bag or pump. This allows the pain medication to be continuously dripped or pumped into the epidural space throughout labor.
There are two main types of epidural setups:
The epidural delivers just one very significant benefit to women in labor – pain relief. Labor and childbirth is painful and the pain and discomfort can last for hours or even days. Aside from the obvious physical discomfort, pain can cause mental stress and anxiety. The epidural is highly effective at eliminating this pain and discomfort.
The reason epidurals are the best method for pain management during childbirth is only the lower body is numbed. This allows the mother to stay awake and mentally alert during delivery. The other critical benefit of having an epidural setup is that the mother’s lower body is already numb which enables doctors to perform an emergency C-section immediately.
If the fetus is oxygen-deprived, time is of the essence to prevent brain damage that can cause cerebral palsy, HIE, or other birth injuries. If an epidural is not in place already, doctors will have to administer a general anesthetic before a C-section. This takes longer and leaves the mother unconscious at birth.
Another possible pro of epidurals is a decreased risk of postpartum depression. Some studies suggest there is strong evidence of lower incidences of depression with an epidural (while others are less convinced).
One initial drawback or limitation with an epidural is that it takes some time and effort and there is only a limited window of time when it can be done. Doctors have to wait until the cervix is at least 4 centimeters dilated before doing an epidural.
Otherwise, the epidural will slow the process down too much. However, once the cervix becomes fully dilated it is too late for an epidural to be given. Another con of the epidural is that inserting the needle into the spine can be quite painful.
There are a handful of known side effects from epidurals that should be listed as cons. Potential negative side effects from an epidural include:
Most mothers will not experience these side effects with an epidural.
Another major drawback of getting an epidural is that it tends to immobilize the mother. With a low dose epidural, the mother may still be able to stand and walk, with help. But at full strength, the medication will completely numb the mother’s lower body and leave her unable to control her legs enough to stand and walk.
The most significant downside of an epidural is that it may prolong the labor and delivery process. The epidural is very effective at numbing the nerves and muscles in a mother’s lower body. The problem is that this makes the mother less able to use her muscles to effectively and rapidly push the baby out.
When the mother is not able to push effectively it prolongs the delivery process and puts the baby under more stress. The longer the delivery process takes more risk there is for a birth injury.
How significant is the increased risk of a birth injury with an epidural? This is where it gets tricky. It is a difficult question. There is not a direct statistic on point. But we do know that epidurals prolong labor. A prolonged delivery increases the risk of an instrumental delivery —vacuum or forceps— or an emergency C-section. Yet few doctors are suggesting an epidural should not be an option. So there are no easy answers. You should digest this page and others like it and then make an informed choice with your OB.
Below are simple answers to some of the most frequently asked questions and concerns that expecting mothers and family have about getting an epidural for pain relief during childbirth.
The singular benefit of an epidural is to decrease the pain of giving birth. The epidural is the most effective form of pain relief during childbirth as it numbs the nerves in the lower half of the mother’s body.
The primary drawback of getting an epidural to reduce pain while giving birth is that it may slow down and prolong the delivery process. The epidural blocks pain by numbing the lower body, but this often reduces the effectiveness of the mother’s efforts to push during contractions.
If the baby’s head is crowning and the doctor or midwife is expecting delivery within in less than 1 hour, it may be too late to get an epidural for pain relief. It takes about 45 minutes to get the epidural catheter in place and for the pain medication to kick in so if the baby is ready to come out soon there won’t be enough time to bother with an epidural.
Hospitals and doctors have their own individual policies for epidurals. In most cases, however, an epidural will not be given until the mother is at least 3-4 centimeters dilated. Once the mother is fully dilated most doctors and hospitals will consider it too late for an epidural to be given.
Once the pain medication stops being administered through the epidural, full sensation should return to the lower body within about 2 hours. It may take longer to feel full control of leg movements when walking.